https://doi.org/10.1140/epjs/s11734-026-02223-z
Regular Article
Non-linear and state-dependent effects of behavioral intervention on glioma progression and survival
1
Shvyrkov Laboratory of Neuronal Bases of Mind, Institute of Psychology, Russian Academy of Sciences, 129366, Moscow, Russia
2
Department of Life Sciences, Moscow Institute of Psychoanalysis, 121170, Moscow, Russia
3
Laboratory of Neuromorphology, Avtsyn Research Institute of Human Morphology of FSBSI Petrovsky National Research Centre of Surgery, 117418, Moscow, Russia
4
Department of Chemistry, Lomonosov Moscow State University, 119991, Moscow, Russia
5
Laboratory of Sleep/Wake Neurobiology, Institute of Higher Nervous Activity and Neurophysiology, Russian Academy of Sciences, 117865, Moscow, Russia
6
Department of Biology, University of Padua, 35121, Padua, Italy
a
This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
30
December
2025
Accepted:
16
February
2026
Published online:
12
March
2026
Abstract
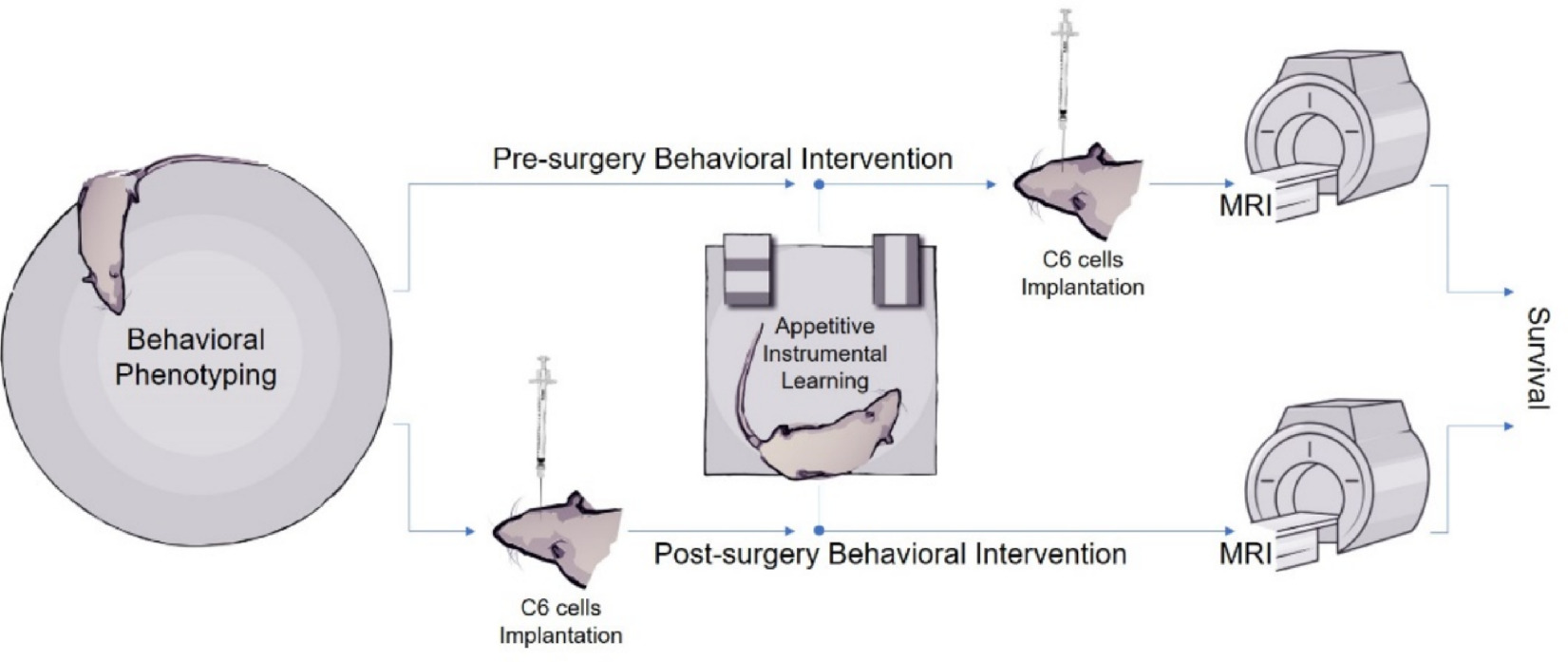
The impact of behavioral interventions on cancer progression is recognized as significant yet poorly understood, with high outcome variability suggesting a key role for individual predispositions. We hypothesize that therapeutic efficacy stems not only from the motor component of an intervention per se, but also from the essential role of positive motivational engagement during learning. Using an intracerebral C6 glioma model in Long–Evans rats, we found that the baseline anxiety level served as a powerful, nonlinear predictor of disease outcome. The highest anxiety scores were associated with the most aggressive tumor growth and the lowest survival. We evaluated how a food-acquisition learning task, administered pre- or post-tumor implantation, modulated this relationship. The intervention attenuated the predictive power of baseline anxiety for tumor progression by improving outcomes in a subset of high-anxiety subjects while worsening them in some with normal anxiety, thereby converging their trajectories. Therefore, failing to account for this nonlinear relationship between baseline anxiety and treatment response can lead to erroneous conclusions in research and to clinical interventions that are, on average, ineffective. Our findings indicate that the outcome of a behavioral intervention—shaped by an individual's psycho-neuro-immune traits and the intervention's motivational context—can remodel the tumor microenvironment. The organism's baseline psychophysiological phenotype sets the initial conditions. A positive motivational context can counteract stress-induced states, leading to a systemic neuroendocrine–immune recalibration that remodels the tumor microenvironment's immune landscape. Thus, we argue for a paradigm shift toward personalized adjuvant strategies based on neuro-immunological profiling, motivated engagement, and controlled stress dynamics.
Copyright comment Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
© The Author(s), under exclusive licence to EDP Sciences, Springer-Verlag GmbH Germany, part of Springer Nature 2026
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.